ASTMH 2018: Session 103 “Unraveling the Biology of the Hypnozoite – Integrating Findings from Lab Models and Field Studies of Plasmodium vivax”
Published: 18/12/2018
Senior editorial support has been facilitated by Graham Brown.
THEMES: THEMES: Basic Science | P. vivax
MESA Correspondents bring you cutting-edge coverage from the 67th ASTMH Annual Meeting
Session 103: “Unraveling the Biology of the Hypnozoite – Integrating Findings from Lab Models and Field Studies of Plasmodium vivax “
This symposium provided an update on the exciting, rapidly emerging technologies that will for the first time enable deeper investigation of the poorly understood liver stages of malaria infection. Ex vivo human liver systems or humanized chimeric mice models supporting development of the hepatic stages of Plasmodium vivax or Plasmodium cynomolgi are now able to be compared with human studies in the field, employing emerging deep sequencing technologies.
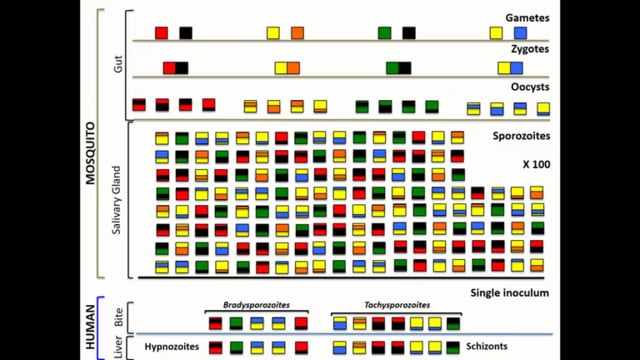
Kevin Baird opened with a stage-setting presentation explaining the Lysenko theory of intrinsic latency phenotypes for relapse behaviours by P. vivax and how that may be tested using modern sequencing technologies applied to laboratory-reared hepatic stages or those of natural infections.
Sandra March described work applying micropatterned co-cultured (MPCC) human hepatocytes supporting the development of liver schizonts and hypnozoites. Whereas primaquine killed both types of parasites, atovaquone selectively killed hepatic schizonts without harming hypnozites. She exploited this treatment to achieve cultures enriched for hypnozoites without schizont co-culture in order to obtain transcriptional profiles of hypnozoites.
Erika Flannery described her work using humanized hepatic chimeric mice to infect those animals. Using sensitive molecular diagnostic methods she confirmed hypnozoite maturation to hepatic schizogony and release of merozoites into blood. The system allowed her to evaluate the killing of hypnozoites during the first 48 hours of development with a single dose of primaquine, a phenomenon observed in human trials a half-century ago.
Jean Popovici described the extraordinary trial involving relocation of 40 patients with Plasmodium vivax from an endemic area of Cambodia to non-endemic Phnom Penh for a period of 60 days follow-up. This allowed exclusion of reinfection as an important and often analytically crippling confounding factor. Though the trial was designed to test for chloroquine resistance in P. vivax, (none was found), Jean exploited the design to examine genotypic relationships between primary and recurrent parasitemias (attributable to true relapse).
Rintis Noviyanti described an essentially similar human trial, but it exploited the movement of heavily exposed Indonesian troops to a non-endemic army base on Java and trials of primaquine therapies. She employed deep sequencing techniques to examine multiplicity of infection among the infections observed, all of which would have been relapses rather than primary attacks. She found that most of the infections (61%) were clonal in nature.
In summary, this session gave a glimpse of how laboratory models, humanized mice, and deep sequencing provide the basic tools for greater understanding of the liver stage of malaria and possible targets for novel interventions.
Co-Chairs: Dr. Jessica Lin (U. North Carolina USA) and Prof. Kevin Baird (U. Oxford Indonesia)
This report was written by Kevin Baird with editorial support from Professor Graham Brown.
Published: 18/12/2018
Senior editorial support has been facilitated by Graham Brown.
THEMES: Basic Science | P. vivax